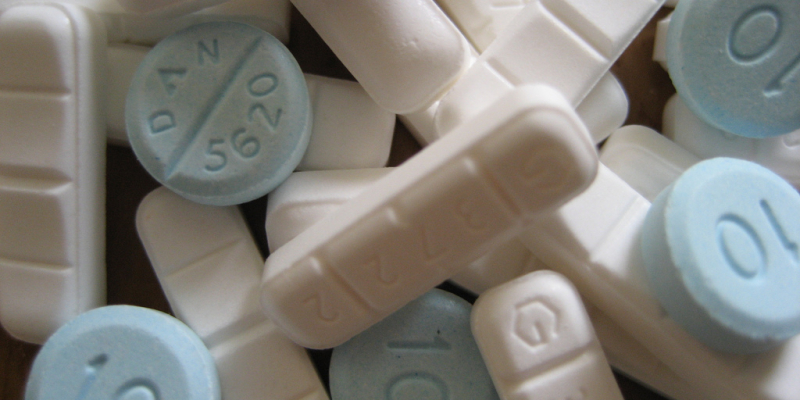
It’s clear that we have a drug epidemic on our hands. Every day you hear of another young soul who lost their battle to addiction. Many times, our assumptions get the best of us. We automatically believe heroin was the culprit. As this is true in many cases, there are so many more where prescription opioids and benzodiazepines are to blame. As it is a well-known fact that both opioids and benzodiazepines can have deadly effects, particularly when used in conjunction with each other, doctors nevertheless continue to prescribe both to patients.
The most recent numbers reveal that 30% of all overdoses have included benzodiazepines. Whether it be Xanax, Valium, or a sister-substance, some form of anxiety medication was found in toxicology screens of overdose victims. Nonetheless, physicians are writing prescriptions for both drugs together at increasing rates. Researchers at Stanford University School of Medicine report, 9% of opioid users also filled a prescription for benzodiazepines in 2001, whereas in 2013, that number increased to 17%.
“Even patients who don’t use ‘heavy’ amounts of opioids are also at higher risk when they also use a benzodiazepine. So physicians should be cautious even with patients who don’t use opioids chronically,” Eric Sun, lead researcher from Stanford University School of Medicine told the Huffington Post. Stanford’s study also determined that if doctors stopped prescribing both opioids and benzodiazepines together, the overdose rate would drop by 15%.
What The Study Found
The study done by Stanford University School of Medicine concluded many findings. Firstly the research was conducted from 2001 to 2013 and analyzed 315,000 privately insured individuals who filled at least one opioid prescription. They found that compared to those that only used opioids, the patients that filled prescriptions for both opioids and benzodiazepines, had more than double the chances of suffering an overdose. Additionally, as one would presume, overdose risks increased dependent upon the frequency of use. Occasional opioid users had a 42% chance of overdose, whereas long-term opioid users were at an 81% risk.
While Sun believes their study to be the first of its kind to analyze opioid-benzodiazepine overdoses, many other studies have been done throughout the country and worldwide, which analyzed the concurrent use of the drugs. In Spain, one study found that 47% of patients in a Methadone clinic found to also be prescribed benzodiazepines, while in a Swiss methadone program, 52% of patients were on a benzo.
As the numbers in this study are disheartening, they only include those who are privately insured. If we were to take into account individuals who are underinsured, not insured whatsoever, or those who have coverage through the state, we would likely see a much higher number. Additionally, if we considered the users who purchase opioids, benzodiazepines, or both illegally, the statistics would surely increase.
The Dangers Of Benzodiazepines & Opioids
“You can imagine that having this breathing drive taken away or severely reduced could lead to serious health consequences. When you hear about people dying from opioid overdose, this is one of the main underlying mechanisms,” Sun remarked.
To better understand how benzos and opioids are a deadly match, one must first know the risks associated with each separately. Benzodiazepines, otherwise known as tranquilizers, are just that. Their initial purpose is to slow things down. Medical experts believe that anxiety and other mental health disorders are often caused by the over-activity in the nerves, and when medicated properly, this excessive amount of activity can be controlled. Researchers found that the GABA neurotransmitter, whose natural function is to calm body, including breathing, can be controlled with benzodiazepines and in turn, so could anxiety disorders. Nevertheless, when used in excess, just like any other chemical that slows the nervous system, an individual can experience drowsiness, slurred speech, lack of coordination, slowed breathing, respiratory distress and/or failure, coma, and death.
Opioids also act on areas within the brain, attaching to receptors and sending signals that would not be there otherwise. Similar to benzodiazepines, opioids send signals of a calming effect, as well as signals that block pain and slow breathing. Furthermore, opioids act on a person’s dopamine levels, also known as the “feel-good” receptor. When an overabundance of dopamine is produced, the individual will experience feelings of euphoria. Opioids can cause drowsiness, slurred speech, slowed breathing, respiratory depression, and death, when taken in high doses….Sound familiar?
Why is it that although we know the risks associated with these medications, especially that of their simultaneous use, doctors will continue to prescribe them in conjunction with each other? We know that each of them can slow an individual’s breathing, sometimes throwing a person into respiratory depression. We also know the likelihood of that happening increases more rapidly when used together, yet opioid users are still able to get their hands on benzo prescriptions. There is simply no excuse anymore. With new measures in place to better assist physicians, such as prescription drug monitoring databases, opioid patients should no longer be able to obtain benzodiazepines as well.
Contact Clearbrook Today
If you or someone you love is struggling with alcoholism or drug addiction, please do not wait any longer. For more than 4 decades, Clearbrook Treatment Centers has been a leader in quality drug and alcohol treatment services. Secluded in the beautiful mountains of northeastern Pennsylvania, you or your loved one will have the opportunity to recover in a peaceful and serene environment. If you are tired of being trapped in the chains of addiction, know there is another way. We have found a solution and would love to share it with you. Take the first step and contact our Admissions Specialists today. We are available 24 hours a day to assist you in any way we can.







